Which Of The Following Physiologic Actions Does Epinephrine Produce
Espiral
Apr 02, 2025 · 6 min read
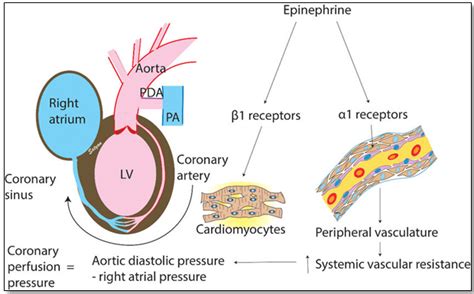
Table of Contents
Which Physiologic Actions Does Epinephrine Produce? A Comprehensive Overview
Epinephrine, also known as adrenaline, is a hormone and neurotransmitter that plays a crucial role in the body's response to stress and danger. Its effects are widespread and profound, impacting numerous physiological systems. Understanding the specific actions of epinephrine is vital for comprehending its role in various physiological processes, as well as its clinical applications and implications. This article delves into the multifaceted physiologic actions of epinephrine, exploring its effects on different organ systems and highlighting the underlying mechanisms.
Cardiovascular System: The Heart of the Matter
Epinephrine's most prominent effects are observed in the cardiovascular system. Its impact on the heart is primarily mediated through the activation of adrenergic receptors, specifically α1, β1, and β2 receptors.
Increased Heart Rate (Chronotropy):
The binding of epinephrine to β1-adrenergic receptors in the heart's sinoatrial (SA) node leads to an increase in the rate of spontaneous depolarization, resulting in a faster heart rate (tachycardia). This is a crucial component of the "fight-or-flight" response, ensuring increased blood flow to vital organs.
Increased Contractility (Inotropy):
Epinephrine also enhances the force of myocardial contraction (positive inotropy). This effect, again mediated through β1-adrenergic receptors, improves the heart's pumping efficiency, increasing cardiac output. This increased contractility ensures that more blood is pumped with each heartbeat, further contributing to the body's response to stress.
Increased Conduction Velocity (Dromotropy):
Epinephrine accelerates the conduction velocity of electrical impulses through the heart's conductive system. This effect, also primarily attributed to β1-adrenergic receptor activation, ensures faster transmission of electrical signals, contributing to the overall increased heart rate and enhanced cardiac output.
Vasoconstriction and Vasodilation: A Balancing Act
Epinephrine's effects on blood vessels are more complex, involving both vasoconstriction and vasodilation, depending on the receptor type and location.
-
Vasoconstriction: Epinephrine binds to α1-adrenergic receptors on vascular smooth muscle, causing vasoconstriction, particularly in the skin, gastrointestinal tract, and kidneys. This shunts blood away from non-essential organs towards the muscles and brain. This effect is particularly important during stressful situations, prioritizing blood flow to organs crucial for survival.
-
Vasodilation: Epinephrine also stimulates β2-adrenergic receptors in skeletal muscle vasculature, leading to vasodilation. This increases blood flow to skeletal muscles, enhancing their ability to respond to the demands of a stressful situation (e.g., running away from danger). This dual effect – vasoconstriction in some areas and vasodilation in others – allows for precise regulation of blood flow to meet the body's immediate needs.
Respiratory System: Breathing Easier Under Pressure
Epinephrine exerts significant effects on the respiratory system, primarily by relaxing bronchial smooth muscle.
Bronchodilation:
The binding of epinephrine to β2-adrenergic receptors in the lungs causes relaxation of bronchial smooth muscle, leading to bronchodilation. This widening of the airways facilitates increased airflow, crucial during situations requiring heightened respiratory effort (e.g., during physical exertion or allergic reactions). This is why epinephrine is a critical component in the treatment of acute asthma attacks.
Increased Respiratory Rate:
While less pronounced than bronchodilation, epinephrine can also indirectly lead to an increased respiratory rate. This effect is likely secondary to other physiological changes, such as increased metabolic rate and oxygen demand.
Metabolic Effects: Fueling the Fight or Flight
Epinephrine's influence extends to the body's metabolic processes, facilitating the mobilization of energy stores to meet the demands of a stressful situation.
Glycogenolysis:
Epinephrine stimulates glycogenolysis, the breakdown of glycogen (stored glucose) into glucose in the liver and skeletal muscles. This process increases blood glucose levels, providing readily available energy for the body's cells. This ensures a surge of glucose is available to power the muscles and brain during the fight-or-flight response.
Lipolysis:
Epinephrine also stimulates lipolysis, the breakdown of fats (triglycerides) into fatty acids in adipose tissue. These fatty acids serve as an alternative energy source, supplementing the glucose released from glycogenolysis. This ensures a sustained energy supply during prolonged periods of stress or exertion.
Gluconeogenesis:
Furthermore, epinephrine can stimulate gluconeogenesis, the synthesis of glucose from non-carbohydrate sources (like amino acids) in the liver. This additional glucose production further contributes to maintaining elevated blood glucose levels during stressful situations.
Other Physiological Effects: A Broader Picture
Beyond its prominent effects on the cardiovascular, respiratory, and metabolic systems, epinephrine influences several other physiological processes:
Central Nervous System: Enhanced Alertness and Focus
Epinephrine enhances alertness and cognitive function, mediating the feeling of heightened awareness and focus characteristic of the fight-or-flight response. This effect is complex and not fully elucidated, but is likely related to its effects on neurotransmitter release and brain activity.
Gastrointestinal Tract: Reduced Activity
Epinephrine reduces gastrointestinal motility and secretions, diverting blood flow away from the digestive system. This is a crucial component of the stress response, as it prioritizes blood flow to vital organs during emergencies. This can manifest as feelings of nausea or a decreased urge to eat during stressful situations.
Immune System Modulation: A Complex Interaction
Epinephrine's effects on the immune system are complex and multifaceted. While it can initially enhance some aspects of immune function, prolonged or excessive exposure can suppress immune responses, contributing to immune dysregulation. This duality is crucial to consider when understanding epinephrine's overall impact on health.
Renal System: Reduced Urine Production
Epinephrine causes vasoconstriction in the renal vasculature, leading to reduced renal blood flow and subsequently decreased urine production. This effect helps maintain blood volume and blood pressure during stressful situations.
Clinical Implications: Therapeutic Uses and Considerations
Understanding the diverse physiological actions of epinephrine is crucial for its appropriate clinical application. It is widely used in various medical settings:
-
Anaphylaxis: Epinephrine is the first-line treatment for anaphylaxis, a severe allergic reaction, primarily due to its potent bronchodilatory and vasoconstricting effects. It helps to counteract the life-threatening effects of allergen-induced bronchospasm and vasodilation.
-
Cardiac Arrest: Epinephrine is used in cardiac arrest to stimulate the heart and increase cardiac output, improving the chances of successful resuscitation.
-
Septic Shock: In septic shock, epinephrine can be used to support blood pressure and improve organ perfusion.
-
Local Anesthesia: Epinephrine is added to local anesthetic solutions to cause vasoconstriction at the injection site, prolonging the anesthetic effect and reducing bleeding.
However, it's crucial to acknowledge that excessive or inappropriate use of epinephrine can have adverse effects, including increased heart rate, palpitations, hypertension, and arrhythmias. Therefore, its use must be carefully managed under medical supervision.
Conclusion: A Powerful Regulator of Physiological Function
Epinephrine is a powerful hormone with profound effects on numerous physiological systems. Its ability to increase heart rate, contractility, and respiratory rate, coupled with its metabolic actions and influence on blood vessel tone, makes it a central component of the body's stress response. Understanding the specific mechanisms of its action is essential for appreciating its vital role in maintaining homeostasis and its various clinical applications. While beneficial in therapeutic settings, its powerful effects require careful consideration and responsible management to avoid potential adverse consequences. Further research continues to expand our knowledge of the intricate and multifaceted roles epinephrine plays in maintaining physiological balance and responding to various physiological demands.
Latest Posts
Latest Posts
-
Do Jumping Spiders Eat Each Other
Apr 03, 2025
-
How Much Was Faron Young Worth When He Died
Apr 03, 2025
-
Vivaldi Composed Approximately How Many Concertos
Apr 03, 2025
-
Islam Is The Oldest Religion In The World
Apr 03, 2025
-
Natural Resources In The Middle Colonies
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about Which Of The Following Physiologic Actions Does Epinephrine Produce . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
